Dracunculiasis
| Dracunculiasis | |
|---|---|
| Other names |
|
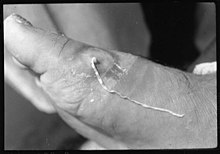 | |
| A D. medinensis worm emerges from a wound on a person's foot | |
| Specialty | Infectious disease |
| Symptoms | Painful blister that a long white worm crawls out of |
| Usual onset | One year after exposure |
| Causes | Ingesting Guinea worm–infected copepods, drinking contaminated water |
| Prevention | Preventing those infected from putting the wound in drinking water, treating contaminated water |
| Treatment | Slowly extracting worm, supportive care |
| Frequency | 14 cases worldwide (2023)[1] |
| Deaths | ~1% of cases |
Dracunculiasis, also called Guinea-worm disease, is a parasitic infection by the Guinea worm, Dracunculus medinensis. A person becomes infected by drinking water contaminated with Guinea-worm larvae that reside inside copepods (a type of small crustacean). Stomach acid digests the copepod and releases the Guinea worm, which penetrates the digestive tract and escapes into the body. Around a year later, the adult female migrates to an exit site – usually the lower leg – and induces an intensely painful blister on the skin. Eventually, the blister bursts, creating a painful wound from which the worm gradually emerges over several weeks. The wound remains painful throughout the worm's emergence, disabling the affected person for the three to ten weeks it takes the worm to emerge.
There is no medication to treat or prevent dracunculiasis. Instead, the mainstay of treatment is the careful wrapping of the emerging worm around a small stick or gauze to encourage and speed up its exit. Each day, a few more centimeters of the worm emerge, and the stick is turned to maintain gentle tension. Too much tension can break and kill the worm in the wound, causing severe pain and swelling. Dracunculiasis is a disease of extreme poverty, occurring in places with poor access to clean drinking water. Prevention efforts center on filtering drinking water to remove copepods, as well as public education campaigns to discourage people from soaking affected limbs in sources of drinking water, as this allows the worms to spread their larvae.
Accounts consistent with dracunculiasis appear in surviving documents from physicians of Greco-Roman antiquity. In the 19th and early 20th centuries, dracunculiasis was widespread across much of Africa and South Asia, affecting as many as 48 million people per year. The effort to eradicate dracunculiasis began in the 1980s following the successful eradication of smallpox. By 1995, every country with endemic dracunculiasis had established a national eradication program. In the ensuing years, dracunculiasis cases have dropped precipitously, with 14 cases reported worldwide in 2023.[1] Since 1986, 14 previously endemic countries have eradicated dracunculiasis, leaving the disease endemic in six: Angola, Central African Republic, Chad, Ethiopia, Mali, and South Sudan. If the eradication program succeeds, dracunculiasis will become the second human disease eradicated, after smallpox. D. medinensis can also infect dogs, cats, and baboons, though animal cases are also falling due to eradication efforts. Other Dracunculus species cause dracunculiasis in reptiles worldwide and in mammals in the Americas.
Cause
[edit]
Dracunculiasis is caused by infection with the roundworm Dracunculus medinensis.[2] D. medinensis larvae reside within small aquatic crustaceans called copepods. Humans typically get infected when they unintentionally ingest copepods while drinking water. In some cases, infected copepods are consumed by fish or frogs, which are then consumed by humans or other animals, passing along the D. medinensis larvae.[3] During digestion the copepods die, releasing the D. medinensis larvae. The larvae exit the digestive tract by penetrating the stomach and intestine, taking refuge in the abdomen or retroperitoneal space (behind the organs near the back of the abdomen).[4] Over the next two to three months the larvae develop into adult male and female worms. The male remains small at 4 cm (1.6 in) long and 0.4 mm (0.016 in) wide; the female is comparatively large, often over 100 cm (39 in) long and 1.5 mm (0.059 in) wide.[5] Once the worms reach their adult size they mate, and the male dies.[6] Over the ensuing months, the female migrates to connective tissue or along bones, and continues to develop.[6]
About a year after the initial infection, the female migrates to the skin, forms an ulcer, and emerges. When the wound touches fresh water, the female spews a milky-white substance containing hundreds of thousands of larvae into the water.[6][7] Over the next several days as the female emerges from the wound, she can continue to discharge larvae into surrounding water.[7] The larvae are eaten by copepods, and after two to three weeks of development, they are infectious to humans again.[8]
Signs and symptoms
[edit]
The first signs of dracunculiasis occur around a year after infection, as the full-grown female worm prepares to leave the infected person's body.[2] As the worm migrates to its exit site – typically the lower leg – some people have allergic reactions, including hives, fever, dizziness, nausea, vomiting, and diarrhea.[6] Upon reaching its destination, the worm forms a fluid-filled blister under the skin.[5] Over 1–3 days, the blister grows larger, begins to cause severe burning pain, and eventually bursts, leaving a small open wound.[2] The wound remains intensely painful as the worm slowly emerges over several weeks to months.[7]
If an affected person submerges the wound in water, the worm spews a white substance releasing its larvae into the water.[5] As the worm emerges, the open blister often becomes infected with bacteria, resulting in redness and swelling; the formation of abscesses; or, in severe cases, gangrene, sepsis, or tetanus.[9][10] When the secondary infection is near a joint (typically the ankle), the damage to the joint can result in stiffness, arthritis, or contractures.[10][11]
Infected people commonly harbor multiple worms – on average 1.8 worms per person,[12] but as many as 40 – which will emerge from separate blisters at the same time.[6] 90% of worms emerge from the legs or feet. However, worms can emerge from anywhere on the body.[6]
Diagnosis
[edit]Dracunculiasis is diagnosed by visual examination – the thin white worm emerging from the blister is unique to this disease.[13] Dead worms sometimes calcify and can be seen in the subcutaneous tissue by X-ray.[10][13]
Treatment
[edit]
There is no medicine to kill D. medinensis or prevent it from causing disease once within the body.[14] Instead, treatment focuses on slowly and carefully removing the worm from the wound over days to weeks.[15] Once the blister bursts and the worm begins to emerge, the wound is soaked in a bucket of water, allowing the worm to empty itself of larvae away from a source of drinking water.[15] As the first part of the worm emerges, it is typically wrapped around a piece of gauze or a stick to maintain steady tension on the worm, encouraging its exit.[15] Each day, several centimeters of the worm emerge from the blister, and the stick is wound to maintain tension.[6] This is repeated daily until the full worm emerges, typically within a month.[6] If too much pressure is applied, the worm can break and die, leading to severe swelling and pain at the site of the ulcer.[6]
Treatment for dracunculiasis also includes regular wound care to avoid infection of the open ulcer. The US Centers for Disease Control and Prevention (CDC) recommends cleaning the wound before the worm emerges. Once the worm begins to exit the body, the CDC recommends daily wound care: cleaning the wound, applying antibiotic ointment, and replacing the bandage with fresh gauze.[15] Painkillers like aspirin or ibuprofen can help ease the pain of the worm's exit.[6][15]
Outcomes
[edit]Dracunculiasis is a debilitating disease, causing substantial disability in around half of those infected.[10] People with worms emerging can be disabled for the three to ten weeks it takes the worms to fully emerge.[10] When worms emerge near joints, inflammation or infection of the affected area can result in permanent stiffness, pain, or destruction of the joint.[10] Some people with dracunculiasis have continuing pain for 12 to 18 months after the worm has emerged.[6] Around 1% of dracunculiasis cases result in death from secondary infections of the wound.[10]
When dracunculiasis was widespread, it often affected entire villages at once.[11] Outbreaks occurring during planting and harvesting seasons severely impaired a community's agricultural operations – earning dracunculiasis the descriptor "empty granary disease" in some places.[11] Communities affected by dracunculiasis also see reduced school attendance as children of affected parents must take over farm or household duties, and affected children may be physically prevented from walking to school for weeks.[16]
Infection does not create immunity, so people can repeatedly experience dracunculiasis throughout their lives.[17]
Prevention
[edit]
There is no vaccine for dracunculiasis, and once infected with D. medinensis there is no way to prevent the disease from running its full course.[14] Consequently, efforts to reduce the burden of dracunculiasis focus on preventing the transmission of D. medinensis from person to person. A mainstay of eradication efforts is the improvement of drinking water. Nylon filters, finely woven cloth, or specialized filter straws can all remove copepods from drinking water, eliminating transmission risk.[6][18] Water sources can also be treated with temephos, which kills copepods,[19] and contaminated water can be treated via boiling.[20] Where possible, open sources of drinking water are replaced by deep wells that can serve as new sources of clean water.[19] Public education campaigns inform people in affected areas how dracunculiasis spreads and encourage those with the disease to avoid soaking their wounds in bodies of water that are used for drinking.[6]
Epidemiology
[edit]Dracunculiasis is now rare, with 14 cases reported worldwide in 2023 and 13 in 2022.[1] This is down from 27 cases in 2020 and dramatically less than the estimated 3.5 million annual cases in 20 countries in 1986 – the year the World Health Assembly called for dracunculiasis's eradication.[21][22] Dracunculiasis remains endemic in three countries: Chad, Mali, and South Sudan.[23]
Dracunculiasis is a disease of extreme poverty, occurring in places where there is poor access to clean drinking water.[24] Cases tend to be split roughly equally between males and females, and can occur in all age groups.[25] Within a given place, dracunculiasis risk is linked to occupation; people who farm or fetch drinking water are most likely to be infected.[25]
When dracunculiasis was widespread, it had a seasonal cycle, though the timing varied by location. Along the Sahara desert's southern edge, cases peaked during the mid-year rainy season (May–October) when stagnant water sources were more abundant.[25] Along the Gulf of Guinea, cases were more common during the dry season (October–March) when flowing water sources dried up.[25]
History
[edit]Diseases consistent with the effects of dracunculiasis are referenced by writers throughout antiquity. Plutarch's Symposiacon refers to a (lost) description by the 2nd century BCE writer Agatharchides concerning a "hitherto unheard-of disease" in which "small worms issue from [people's] arms and legs ... insinuating themselves between the muscles [to] give rise to horrible sufferings".[26] Greco-Roman and Persian physicians, including Galen, Rhazes, and Avicenna, also wrote of diseases consistent with dracunculiasis; though there was some disagreement as to the nature of the disease, with some attributing it to a worm, while others considered it to be a corrupted part of the body emerging.[26]
Some have proposed links between dracunculiasis and other prominent ancient texts and symbols. In a 1674 treatise on dracunculiasis, Georg Hieronymous Velschius ascribed serpentine figures in several ancient icons to Dracunculus, including Greek sculptures, signs of the zodiac, Arabic lettering, and the Rod of Asclepius, a common symbol of the medical profession.[26] Similarly, parasitologist Friedrich Küchenmeister proposed in 1855 that the "fiery serpents" that plague the Hebrews in the Old Testament represented dracunculiasis.[26][note 1] In 1959, parasitologist Reinhard Hoeppli proposed that a prescription in the Ebers papyrus – a medical text written around 1500 BCE – referred to the removal of a Guinea worm, an identification endorsed ten years later by the physician and Egyptologist Paul Ghalioungui; this would make the Ebers papyrus the oldest known description of the disease.[note 2][29]
Carl Linnaeus included the Guinea worm in his 1758 edition of Systema Naturae, naming it Gordius medinensis.[26] The name medinensis refers to the worm's longstanding association with the Arabian Peninsula city of Medina, with Avicenna writing in his The Canon of Medicine (published in 1025) "The disease is commonest at Medina, whence it takes its name".[26] In Johann Friedrich Gmelin's 1788 update of Linnaeus' Systema Naturae, Gmelin renamed the worm Filaria medinensis, leaving Gordius for free-living worms.[26] Henry Bastian authored the first detailed description of the worm itself, published in 1863.[26][30] The following year, in his book Entozoa, Thomas Spencer Cobbold used the name Dracunculus medinensis, which was enshrined as the official name by the International Commission on Zoological Nomenclature in 1915.[26] Despite longstanding knowledge that the worm was associated with water, the lifecycle of D. medinensis was the topic of protracted debate.[31] Alexei Pavlovich Fedchenko filled a major gap with his 1870 publication describing that D. medinensis larvae can infect and develop inside copepods.[32][33][note 3] The next step was shown by Robert Thomson Leiper, who described in a 1907 paper that monkeys fed D. medinensis–infected copepods developed mature Guinea worms, while monkeys directly fed D. medinensis larvae did not.[32]
In the 19th and 20th centuries, dracunculiasis was widespread across nearly all of Africa and South Asia, though no exact case counts exist from the pre-eradication era.[25] In a 1947 article in the Journal of Parasitology, Norman R. Stoll used rough estimates of populations in endemic areas to suggest that there could have been as many as 48 million cases of dracunculiasis per year.[34][35] In 1976, the WHO estimated the global burden at 10 million cases per year.[35] Ten years later, as the eradication effort was beginning, the WHO estimated 3.5 million cases per year worldwide.[36]
Eradication
[edit]
The campaign to eradicate dracunculiasis began at the urging of the CDC in 1980.[37] Following smallpox eradication (last case in 1977; eradication certified in 1981), dracunculiasis was considered an achievable eradication target since it was preventable with only behavioral changes and less common than many similar diseases of poverty.[38] In 1981, the steering committee for the United Nations International Drinking Water Supply and Sanitation Decade (a program to improve global drinking water from 1981 to 1990) adopted the goal of eradicating dracunculiasis as part of their efforts.[39] The following June, an international meeting termed "Workshop on Opportunities for Control of Dracunculiasis" concluded that dracunculiasis could be eradicated through public education, drinking water improvement, and larvicide treatments.[39] In response, India began its national eradication program in 1983.[39]
In 1986, the 39th World Health Assembly issued a statement endorsing dracunculiasis eradication and calling on member states to craft eradication plans.[38] The same year, the Carter Center began collaborating with the government of Pakistan to initiate its national program, which then launched in 1988.[39] By 1996, national eradication programs had been launched in every country with endemic dracunculiasis: Ghana and Nigeria in 1989; Cameroon in 1991; Togo, Burkina Faso, Senegal, and Uganda in 1992; Benin, Mauritania, Niger, Mali, and Côte d'Ivoire in 1993; Sudan, Kenya, Chad, and Ethiopia in 1994; Yemen and the Central African Republic in 1995.[38][40]
Each national eradication program had three phases. The first phase consisted of a nationwide search to identify the extent of dracunculiasis transmission and develop national and regional plans of action. The second phase involved the training and distribution of staff and volunteers to provide public education village-by-village, surveil for cases, and deliver water filters. This continued and evolved as needed until the national burden of disease was very low. Then, in a third phase, programs intensified surveillance efforts with the goal of identifying each case within 24 hours of the worm emerging and preventing the person from contaminating drinking water supplies. Most national programs offered voluntary in-patient centers, where those affected could stay and receive food and care until their worms were removed.[41]
In May 1991, the 44th World Health Assembly called for an international certification system to verify dracunculiasis eradication country-by-country.[39] To this end, in 1995 the WHO established the International Commission for the Certification of Dracunculiasis Eradication (ICCDE).[42] Once a country reports zero cases of dracunculiasis for a calendar year, the ICCDE considers that country to have interrupted Guinea worm transmission, and is then in the "precertification phase".[43] If the country reports zero cases in each of the next three calendar years, the ICCDE sends a team to the country to assess the country's disease surveillance systems and to verify the country's reports.[43] The ICCDE can then formally recommend the WHO Director-General certify a country as free of dracunculiasis.[42]
Since the initiation of the global eradication program, the ICCDE has certified 15 of the original endemic countries as having eradicated dracunculiasis: Pakistan in 1997; India in 2000; Senegal and Yemen in 2004; the Central African Republic and Cameroon in 2007; Benin, Mauritania, and Uganda in 2009; Burkina Faso and Togo in 2011; Côte d'Ivoire, Niger, and Nigeria in 2013; and Ghana in 2015.[23] In 2020, the 76th World Health Assembly endorsed a new guidance plan, the Roadmap for Neglected Tropical Diseases 2021–2030, which sets a 2027 target for eradication of dracunculiasis, allowing certification by the end of 2030.[44]
Other animals
[edit]In addition to humans, D. medinensis can infect domestic dogs and cats and wild olive baboons.[45] Infections of domestic dogs have been particularly common in Chad, where they helped reignite dracunculiasis transmission in 2010.[46] Animals are thought to become infected by eating a transport host, likely a fish or amphibian.[47] As with humans, control efforts have focused on preventing infection by encouraging people in affected areas to bury fish entrails, as well as to identify and tie up dogs and cats with emerging worms so that they cannot access drinking water sources until after the worms have emerged.[47] Animal infections are rapidly falling, with 2,000 recorded infections in 2019, 1,601 in 2020, and 863 in 2021.[48][49] Domestic ferrets can be infected with D. medinensis in laboratory settings, and have been used as an animal disease model for human dracunculiasis.[50]
Other Dracunculus species can infect snakes, turtles, and other mammals. Animal infections are most widespread in snakes, with nine different species of Dracunculus described in snakes in the United States, Brazil, India, Vietnam, Australia, Papua New Guinea, Benin, Madagascar, and Italy.[51][52] The only other reptiles affected are snapping turtles, with cases of infected common snapping turtles described in several US states and a single infected South American snapping turtle described in Costa Rica.[53] Infections of other mammals are limited to the Americas. Raccoons in the US and Canada are most widely impacted, particularly by D. insignis; however, Dracunculus worms have also been reported in American skunks, coyotes, foxes, opossums, domestic dogs, domestic cats, and (rarely) muskrats and beavers.[54][55]
Notes
[edit]- ^ This theory was criticised at the time, with The British Medical Journal's book review pointing out differences in the disease's incubation time and fatality making it a poor match for the Book of Numbers description.[27][26]
- ^ Ghalioungui translates Ebers No. 875 thus:[28]
If you examine a swelling ... on any body-part of man, you must apply thereon a bandage; and if you find it coming and going and clinging to the flesh which is under it ... You must perform a knife treatment, cutting it out with a ds-knife and that which is in its interior is seized with the hnw-instrument ... You must then extirpate it with the ds-knife ... It shall be seized with the hnwjt-part of any colocynch. A swelling that is like a head is to be treated likewise.
- ^ Fedchenko suggested that this discovery was serendipitous based on his observations of many waterborne animals. However, Rudolf Leuckart claimed that he had advised Fedchenko to investigate Cyclops copepods due to the similarity between D. medinensis and the fish parasite Cucullanus elegans, the life cycle of which Leuckart had described in 1865.[32]
References
[edit]- ^ a b c "Update: 14 human cases of Guinea worm reported in 2023". The Carter Center. 6 March 2024. Archived from the original on 10 March 2024. Retrieved 19 April 2024.
- ^ a b c "Guinea worm disease frequently asked questions". US Centers for Disease Control and Prevention. 11 August 2023. Archived from the original on 28 May 2023. Retrieved 8 August 2022.
- ^ Hopkins et al. 2022, "Chad".
- ^ "Dracunculiasis – DPDx". US Centers for Disease Control and Prevention. 9 May 2018. Archived from the original on 23 January 2023. Retrieved 27 April 2024.
- ^ a b c Despommier et al. 2019, p. 287.
- ^ a b c d e f g h i j k l m Spector & Gibson 2016, p. 110.
- ^ a b c Hotez 2013, p. 67.
- ^ Despommier et al. 2019, pp. 287–288.
- ^ "Guinea worm – disease". US Centers for Disease Control and Prevention. 4 February 2022. Archived from the original on 22 August 2022. Retrieved 8 August 2022.
- ^ a b c d e f g Despommier et al. 2019, p. 288.
- ^ a b c Hotez 2013, p. 68.
- ^ Greenaway 2004, "Clinical manifestations".
- ^ a b Marie C, Petri WA (September 2022). "Dracunculiasis". Merck & Co. Archived from the original on 26 April 2021. Retrieved 27 April 2024.
- ^ a b "Dracunculiasis (Guinea-worm disease)". World Health Organization. 10 January 2022. Archived from the original on 17 October 2019. Retrieved 27 April 2024.
- ^ a b c d e "Management & Treatment". US Centers for Disease Control and Prevention. 4 February 2022. Archived from the original on 7 February 2023. Retrieved 27 April 2024.
- ^ Ruiz-Tiben & Hopkins 2006, Section 4.2 "Socio-Economic Impact".
- ^ Callahan et al. 2013, Introduction.
- ^ Despommier et al. 2019, p. 289.
- ^ a b Spector & Gibson 2016, p. 111.
- ^ "Control of Neglected Tropical Diseases". World Health Organization. Archived from the original on 7 December 2023. Retrieved 6 December 2023.
- ^ WHO 2022, Figure 1.
- ^ Despommier et al. 2019, p. 285.
- ^ a b "Year in which countries certified". World Health Organization. Archived from the original on 21 October 2021. Retrieved 20 October 2021.
- ^ Spector & Gibson 2016, p. 109.
- ^ a b c d e Ruiz-Tiben & Hopkins 2006, Section 4. "Epidemiology".
- ^ a b c d e f g h i j Grove 1990, pp. 693–698.
- ^ "Reviews and notices – the diseases of the Bible". The British Medical Journal. 2 (1406): 1283–1284. December 1887.
- ^ Ghalioungui P (1987). The Ebers Papyrus: a new English translation, commentaries, and glossaries. Cairo: Academy of Scienctific Research and Technology. p. 253. OCLC 25868848.
- ^ Miller 1989, p. 251.
- ^ Bastian HC (November 1863). "On the structure and nature of the Dracunculus, or Guinea worm". Transactions of the Linnean Society of London. 24 (2): 101–134. doi:10.1111/j.1096-3642.1863.tb00155.x. Archived from the original on 25 January 2023. Retrieved 13 June 2022.
- ^ Grove 1990, pp. 698–702.
- ^ a b c Grove 1990, pp. 702–706.
- ^ Fedchenko A (1870). "О строении и размножении ришты (Filaria medinensis L.)" [On the structure and reproduction of the Guinea worm (Filaria medinensis L.)]. Известия Императорского Общества Любителей Естествознания, Антропологии и Этнографии [News of the Imperial Society of Devotees of Natural Science, Anthropology and Ethnography (Moscow)] (in Russian). 8 (1): 71–82. English translation: Fedchenko AP (1971). "Concerning the structure and reproduction of the Guinea-worm (Filaria medinensis L.)". American Journal of Tropical Medicine and Hygiene. 20 (4): 511–523. doi:10.4269/ajtmh.1971.20.511.
- ^ Stoll NR (February 1947). "This wormy world". Journal of Parasitology. 33 (1): 1–18. JSTOR 3273613. PMID 20284977.
- ^ a b Biswas et al. 2013, "Decision to Eradicate".
- ^ "Dracunculiasis – global surveillance summary, 1" (PDF). Weekly Epidemiological Record (19). World Health Organization. 10 May 1996. OCLC 194592343. Archived (PDF) from the original on 3 June 2022. Retrieved 2 June 2022.
- ^ Hopkins et al. 2018, Introduction.
- ^ a b c Hotez 2013, p. 69.
- ^ a b c d e Ruiz-Tiben & Hopkins 2006, Section 5. "Eradication Campaign".
- ^ Ruiz-Tiben & Hopkins 2006, Table 1.
- ^ Ruiz-Tiben & Hopkins 2006, Section 5.7 "Strategy for Eradication".
- ^ a b Biswas et al. 2013, Section "Certification of eradication".
- ^ a b "International commission for the certification of dracunculiasis eradication – about us". World Health Organization. Archived from the original on 5 September 2021. Retrieved 5 September 2021.
- ^ Hopkins et al. 2022, "Introduction".
- ^ Hopkins et al. 2022, "Ethiopia".
- ^ Eberhard et al. 2014, "Abstract".
- ^ a b Molyneux & Sankara 2017, Paragraph 7.
- ^ Hopkins et al. 2021, "Table 1".
- ^ Hopkins et al. 2022, "Current status of the campaign".
- ^ Cleveland et al. 2018, "Experimental infections of hosts with D. insignis".
- ^ Cleveland et al. 2018, "Table 1".
- ^ Cleveland et al. 2018, "Dracunculus species of squamates".
- ^ Cleveland et al. 2018, "Dracunculus species in chelonians".
- ^ Cleveland et al. 2018, "Natural infections of D. insignis in wildlife".
- ^ Cleveland et al. 2018, ""Dracunculus species in mammals".
Works cited
[edit]- Biswas G, Sankara DP, Agua-Agum J, Maiga A (August 2013). "Dracunculiasis (Guinea worm disease): eradication without a drug or a vaccine". Philosophical Transactions of the Royal Society B. 368 (1623): 20120146. doi:10.1098/rstb.2012.0146. PMC 3720044. PMID 23798694.
- Callahan K, Bolton B, Hopkins DR, Ruiz-Tiben E, Withers PC, Meagley K (30 May 2013). "Contributions of the Guinea Worm Disease eradication campaign toward achievement of the Millennium Development Goals". PLOS Neglected Tropical Diseases. 7 (5): e2160. doi:10.1371/journal.pntd.0002160. PMC 3667764. PMID 23738022.
- Cleveland CA, Garrett KB, Cozad RA, Williams BM, Murray MH, Yabsley MJ (December 2018). "The wild world of Guinea Worms: A review of the genus Dracunculus in wildlife". International Journal for Parasitology: Parasites and Wildlife. 7 (3): 289–300. doi:10.1016/j.ijppaw.2018.07.002. PMC 6072916. PMID 30094178.
- Despommier DD, Griffin DO, Gwadz RW, Hotez PJ, Knirsch CA (2019). "25. Dracunculus medinensis". Parasitic Diseases (PDF) (7 ed.). Parasites Without Borders. pp. 285–290. Archived (PDF) from the original on 24 November 2021. Retrieved 26 January 2021.
- Eberhard ML, Ruiz-Tiben E, Hopkins DR, Farrell C, Toe F, Weiss A, Withers PC, Jenks MH, Thiele EA, Cotton JA, Hance Z, Holroyd N, Cama VA, Tahir MA, Mounda T (January 2014). "The peculiar epidemiology of dracunculiasis in Chad". American Journal of Tropical Medicine and Hygiene. 90 (1): 61–70. doi:10.4269/ajtmh.13-0554. PMC 3886430. PMID 24277785.
- Greenaway C (February 2004). "Dracunculiasis (Guinea worm disease)". Canadian Medical Association Journal. 170 (4): 495–500. PMC 332717. PMID 14970098.
- Grove DI (1990). A History of Human Helminthology (PDF). C.A.B International. Archived (PDF) from the original on 4 April 2015. Retrieved 13 March 2022.
- Hopkins DR, Ruiz-Tiben E, Eberhard ML, Weiss A, Withers PC, Roy SL, Sienko DG (August 2018). "Dracunculiasis eradication: are we there yet?". American Journal of Tropical Medicine and Hygiene. 99 (2): 388–395. doi:10.4269/ajtmh.18-0204. PMC 6090361. PMID 29869608.
- Hopkins DR, Weiss AJ, Roy SL, Yerian S, Cama VA (November 2021). "Progress toward global eradication of dracunculiasis, January 2020–June 2021". Morbidity and Mortality Weekly Report. 70 (44): 1527–1533. doi:10.15585/mmwr.mm7044a1. PMC 8568094. PMID 34735420.
- Hopkins DR, Weiss AJ, Torres-Velez FJ, Sapp SG, Ijaz K (August 2022). "Dracunculiasis eradication: end-stage challenges". American Journal of Tropical Medicine and Hygiene. 107 (2): 373–382. doi:10.4269/ajtmh.22-0197. PMC 9393450. PMID 35895421.
- Hotez PJ (2013). "The filarial infections: lymphatic filariasis (elephantiasis) and dracunculiasis (Guinea worm)". Forgotten People, Forgotten Diseases: The Neglected Tropical Diseases and Their Impact on Global Health and Development. American Society for Microbiology (ASM) Press. pp. 57–75.
- Miller RL (1989). "Dqr, spinning and treatment of Guinea worm in P. Ebers 875". The Journal of Egyptian Archaeology. 75: 249–254. doi:10.2307/3821922. JSTOR 3821922.
- Molyneux D, Sankara DP (April 2017). "Guinea worm eradication: Progress and challenges— should we beware of the dog?". PLOS Neglected Tropical Diseases. 11 (4): e0005495. doi:10.1371/journal.pntd.0005495. PMC 5398503. PMID 28426663.
- Ruiz-Tiben E, Hopkins DR (2006). "Dracunculiasis (Guinea worm disease) eradication". Advances in Parasitology. 61: 275–309. doi:10.1016/S0065-308X(05)61007-X. ISBN 9780120317615. PMID 16735167.
- Spector JM, Gibson TE, eds. (2016). "Dracunculiasis". Atlas of Pediatrics in the Tropics and Resource-Limited Settings (2 ed.). American Academy of Pediatrics. pp. 109–115. ISBN 978-1-58110-960-3.
- Dracunculiasis eradication: global surveillance summary, 2021 (Report). World Health Organization. 27 May 2022. Archived from the original on 29 July 2022. Retrieved 29 July 2022.
